Bone Density Test
A bone density test (also known as bone densitometry) uses a very low-dose X-ray machine that evaluates bone loss commonly associated with osteopenia or osteoporosis. Sometimes, physicians or patients will refer to a bone density test as a BMD (bone mineral density) scan or DEXA scan. The bone density test uses two low-energy X-ray beams to scan the strength of your bones, identify and test potential fracture risk, and evaluate the efficacy of therapy.
Bone Density Tests
in Alberta
With Testing Locations in Edmonton, Fort McMurray, Leduc, Sherwood Park, St. Albert, & Spruce Grove
A bone density test, also known as BMD (bone mineral density), DEXA, or bone densitometry exam, is most commonly performed on the lumbar spine, hip, and forearm, as these bones have been shown to generate the most reliable measurements for predicting fractures and monitoring treatment.
These exams are also used to measure calcium levels, bone loss, and bone structure fragility. By measuring the bone mineral content or density of your bones, doctors can predict whether or not you may be at risk for fractures and can recommend treatment right away.
Osteoporosis Canada recommends bone density testing and spinal x-rays as part of their world-class Fracture Liaison Service model. Additionally, these three bone density imaging locations are the basis of the World Health Organization’s algorithm for predicting risk factors in the assessment of osteoporosis.
The radiation dose from a density test is minimal and is similar to the exposure you get when you go through an airport security scan.
Who Benefits From a Bone Density Diagnostic Exam
- Both men and women over age 65
- Post-menopausal women 50 or older with additional risk factors
- Men 50 or older with additional risk factors
Who Qualifies For a Bone Density Diagnostic Exam
Patients 50+
- Are eligible to have a bone density exam once every 2 years
- 50+-year-old patients who had a bone density test done less than 2 years ago (anywhere in Alberta) must meet one or more of the clinical indications below before a bone density exam can be performed:
- On Osteoporosis medication that has been started since the last exam
- On Oral steroid medication – any dose taken longer than 12 months
- Patient being monitored during a “bisphosphonate holiday” – e.g. Patient has been on osteoporosis drugs and now off for more than 1 year
- Patient on therapy in whom there are clinical features to question drug effect
- Patient has hyperparathyroidism
- Cancer or transplant patient
- Radiologist has recommended a one-year follow-up on prior exam
Patients Under 50
- Must have a referral from one of these specialists:
- Endocrinologist
- Gastroenterologist
- General Surgeon
- Internal Medicine
- Nephrology
- Orthopedic
- Physical Medicine and Rehab
- Rheumatology
- Pediatrician
- Gynecology Oncologist (Cross Cancer)
- Radiologist has recommended a one-year follow-up on a previous report
Cost
Patients that are not eligible to have a Bone Density exam based on the criteria above, but have a requisition, can pay for the exam if they request it.
The cost for a bone density test is $152.
If you fit into any of the following categories, you are also at risk of developing low bone mineral density and should consult with your doctor as soon as possible:
- Early menopause
- Poor physical health
- Any spinal or hip fracture
- High alcohol or smoking intake
- Low body weight (less than 132 pounds)
- Fracture from standing height or less after age 40
- Intake of medications such as glucocorticoids or hormone blockers
- Poor diet that lacks in adequate amounts of vitamins and calcium intake
- Conditions such as rheumatoid arthritis, Cushing’s disease, malabsorption syndrome, hyperparathyroidism, or chronic inflammatory conditions
Detecting Osteoporosis with Bone Density Tests
The information acquired from these diagnostic exams is incredibly useful for physicians when determining if a patient has osteoporosis, osteopenia, or is at risk for future compromised bone structure.
It’s important to educate yourself about bone loss symptoms, exercises, and treatment to help prevent the degradation of your body and bones.
There are 2 different types of bone densitometry exams depending on the area of concern. Central DEXA (or Dual Energy X-ray Absorptiometry) examines your hip bones and spinal area, while peripheral tests examine the bone density levels present in your wrist, finger, and heel zones.
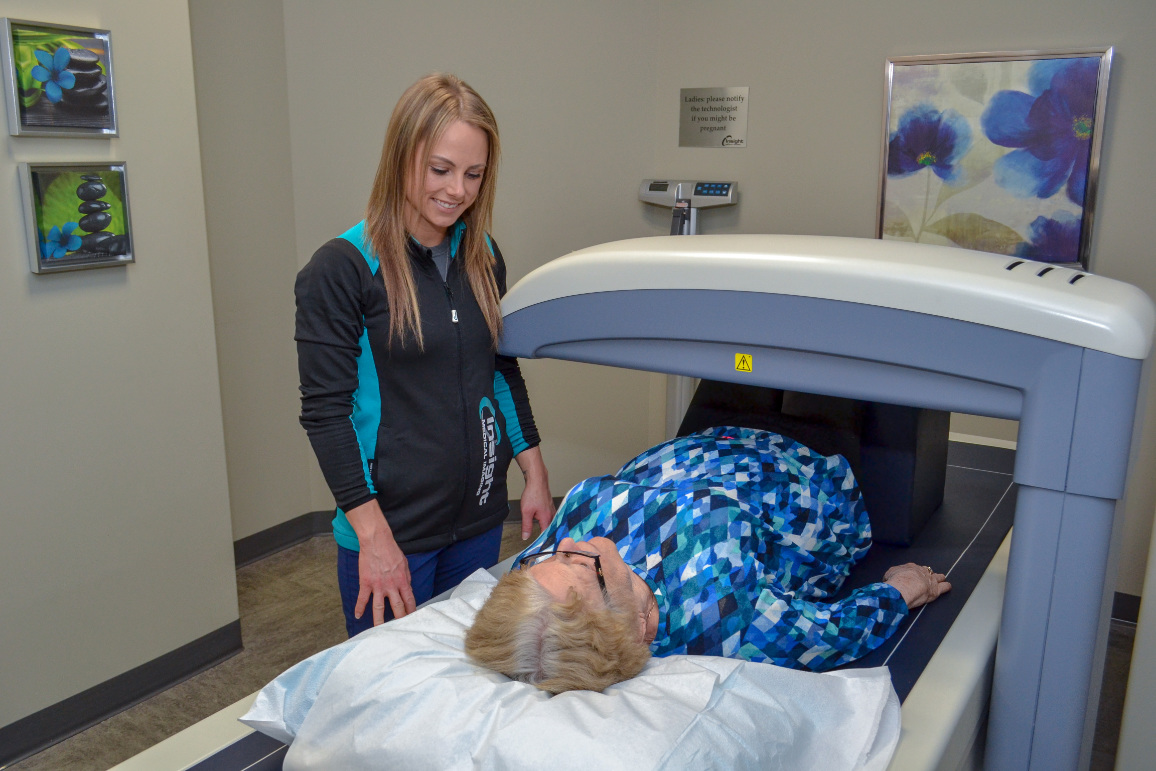
What To Expect
At the time of booking your testing, you will be asked to wear clothing that does not contain any metals such as snaps, buttons, or zippers. As this is crucial to ensuring quality imaging results, you also may be asked to change into a gown when you arrive to further ensure there are no metals on your person.
You will be weighed and your height measured before your scan. Our scanning beds have a maximum weight restriction of 300 pounds. If you exceed the 300-pound weight limit of the machine, we will position you beside the scanner with your arm extended outwards.
Before your testing, you will be positioned on a bed by our technologist. We will use a foam block to elevate your legs in an upright position to align the spine for optimal measurements.
The scan should take approximately 10 minutes. Please remain as still as possible as movement may blur the images.
Using dual-energy x-ray absorptiometry, we will calculate your bone mineral content. If there is any chance that you are pregnant, please talk to your doctor before coming in for your scan.
Depending on your exam, a scanner will pass over you and examine your lower spine or hip. If we’re completing the modified version of the test, we will scan your wrist.
After the scan is complete, one of our bone density radiologists will review the results and send a detailed report to your doctor.
Important Patient Information
All scans use ionizing radiation. Therefore, there must be zero chance a patient is pregnant. We ask all patients between 11 and 55 years of age about their last menstrual cycle to determine the possibility of pregnancy.
We understand that this information may be uncomfortable to share with others — we ask this personal question to protect a fetus from radiation exposure. If there is any chance you are pregnant, please tell your doctor before coming to your DEXA/bone density scan.
In addition, recent changes by the Government of Alberta to the Schedule of Medical Benefits (SOMB) Health Service Code X128 state that patients seeking a bone mineral densitometry scan are only allowed to have one scan every two years.
Patients considered “high risk” for osteoporosis may have BMD scans done more frequently when referred by a specialist. Special cases include endocrinology, metabolism, gastroenterology, surgery, internal medicine, nephrology, orthopedic, pediatric, and rheumatology.
Understanding Your Bone Density Exam Scores
A bone density test will provide you with a T-score and a Z-score.
For adults 50 years and older, the bone mineral density classification will be determined using the lowest T-score on the test for the lumbar spine, hip, neck, radius, and total body. If the T-score is greater than or equal to -1.0, you have normal bone mass. If the T-score is between -1.0 and -2.5, you have low bone mass (osteopenia). If the T-score is less than or equal to -2.5, you likely have osteoporosis.
For adults 18 to 49 years, the classification will be determined using the lowest Z-score. Our radiologist will compare this Z-score to a statistical average for the appropriate age group.
A Z-score alone is not used to diagnose osteoporosis or osteopenia, but it does provide valuable insights for patients and physicians. Patients with Z-scores above -2.0 are considered to have normal bone density. If your Z-score is -2.0 or lower on the test, your bone density is below the statistical average.
Your physician will use the testing results and other clinical risk factors to determine your 10-year bone fracture risk (FRAX).
Exam Cost
If you have an Alberta or a valid out-of-province health care card, your bone density test comes at no cost (except for Quebec). Residents of Quebec may have a portion of their health care reimbursed by the RAMQ.
Bone Density Test vs. Bone Scan
There are many different names for a bone mineral densitometry scan. The most common names for this exam include bone (mineral) density tests, BMD, and DEXA/ DXA exams. All of these names refer to the same diagnostic imaging scan. Sometimes ‘DEXA’ or ‘DXA’ is used for a body composition scan, as both exams typically use the same x-ray technology.
However, these exams are not to be confused with a bone scan. While the term ‘bone scan’ is very close to all the previously listed names, it is in fact a very different type of diagnostic imaging test. A bone scan is a nuclear medicine test that involves injecting a radiopharmaceutical into the body, which is later scanned to form diagnostic images. These radioisotopes travel through your body and accumulate at imperfections in the bones. A specialized diagnostic scanning machine pinpoints isotope accumulations, which are indicative of bone microfractures.
In a bone density test, radiation emission originates from the scanner. Conversely, radiopharmaceutical injections used in a bone scan emit radiation from inside the body, after the injection. The purpose of a bone density test is to measure how porous or dense the bones in your body are. It is not meant to find microfractures like a bone scan. Patients often confuse the two exams when checking in with our receptionists or booking with our patient care coordinators. While the requisition provided by your physician should tell us precisely what test to perform, sometimes mistakes are made when completing a referral.
When a patient is adamant that they are supposed to get a specific imaging test, our reception team may phone the referring physician’s office to confirm everything before proceeding. Calling the referring physician is an important step, as it ensures we are performing the right diagnostic imaging test. While the exam preparation for both tests is the same, we must not confuse the two scans, as both tests have very different goals. We also don’t want to waste anyone’s time – yours, the technologist’s, or your referring physician’s.
Most importantly, we want to adhere to ALARA principles and ensure we are not exposing you to unnecessary radiation.
What Happens After Your Bone Densitometry Exam
It is important to note that no matter your results, you have options available. If you have low bone mass, it is commonly recommended that you increase your weight-bearing exercise and focus on your nutrition. Specifically, ensure you are getting enough vitamin D and calcium. For a complete guide, visit the National Osteoporosis Foundation's website for more information on calcium and vitamin D recommendations for osteoporosis.
If the results of your bone density test show that you have osteoporosis, your physician may prescribe a medication to reduce bone breakdown. It is also crucial that you make lifestyle changes, similar to what those impacted by osteopenia must do.
Clinics that Offer Bone Density Testing:
- 2460 Guardian Rd NW Edmonton, AB, T5T 1K8
- 780-486-8132
- Mon- Fri 7:30 am - 4:00 pm
- 110, 75 Neil Ross Rd St. Albert, AB T8N 7W1
- 780-438-3802
- Monday - Friday: 7:30 AM - 4:00 PM
- 15309 Castle Downs Rd NW Edmonton, AB T5X 6C3
- 780-457-4070
- Monday - Friday: 7:30 AM - 4:00 PM Extended Hours: Monday - Friday: 4:00 PM - 8:00 PM Saturday: 9:00 AM - 5:00 PM
- 1 - 606 Signal Road - Westwood Plaza Fort McMurray, AB T9H 4Z4
- 780-791-1992
- Monday - Friday: 7:30 AM - 4:00 PM
- 2049 111 ST NW Edmonton, AB T6J 4V9
- 780-438-0547
- Monday - Friday: 7:30 AM - 4:00 PM Extended Hours: Monday - Friday: 4:00 PM - 8:00 PM Saturday: 9:00 AM - 5:00 PM
- 12779 50 ST NW Edmonton, AB T5A 4L8
- 780-475-1866
- Monday - Friday: 7:30 AM – 4:00 PM Extended Hours: Monday - Friday: 4:00 PM - 8:00 PM Saturday: 9:00 AM - 5:00 PM
- 5307 50 AVE Leduc, AB T9E 6T2
- 780-486-8104
- Monday - Friday: 7:30 AM - 4:00 PM
- 10381 51 AVE NW Edmonton, AB T6H 0K4
- 780-434-9171
- Monday - Friday: 7:45 AM - 4:00 PM
- 200 Meadowlark Shopping CTR NW Edmonton, AB T5R 5W9
- 780-489-8430
- Monday - Friday: 7:30 AM - 4:00 PM
- 6466 28 AVE NW Edmonton, AB T6L 6N3
- 780-486-8103
- Monday - Friday: 7:30 AM - 4:00 PM Extended Hours: Monday - Friday: 4:00 PM - 8:00 PM Saturday: 9:00 AM - 5:00 PM
- 136 Athabascan AVE Sherwood Park, AB T8A 4E3
- 780-464-1515
- Monday - Friday: 7:30 AM - 4:00 PM Extended Hours: Monday - Friday: 4:00 PM - 8:00 PM Saturday: 9:00 AM - 5:00 PM
- 107-505 Queen ST Spruce Grove, AB T7X 2V2
- 780-962-0297
- Monday - Friday: 7:30 AM - 4:00 PM Extended Hours: Monday: 4:00 PM - 8:00 PM Wednesday: 4:00 PM - 8:00 PM Thursday: 4:00 PM - 8:00 PM
- 11560 104 AVE NW Edmonton, AB T5K 2S5
- 780-486-8102
- Monday - Friday: 7:30 AM - 4:00 PM
Exam Preparation
Planning your next appointment? Learn more about bone density test preparation and find the medical imaging clinic most convenient for you.